The DNA of fighting pandemics: cloned against coronavirus
Developing optimal policies to fight pandemics and COVID-19 combat in the United States.
By Eyüp Çetin, Serap Kiremitci and Barış Kiremitci
May 17, 2020
The world has faced an important number of outbreaks and pandemics with death tolls of hundreds of millions throughout its history. A novel coronavirus (2019-nCoV or SARS-CoV-2) was first publicized from Wuhan, China, on 31 December 2019 as a new strain [1].
The Virus Goes Viral
As number of infected countries grows, the WHO defined the COVID-19 outbreak as a pandemic on 11 March 2020. It is the first pandemic caused by a coronavirus and the first pandemic which is also controllable [2]. WHO Risk Assessment is currently “Very High” at Global Level as of 16 May 2020 03:00 GMT+3, there are 4,396,392 globally confirmed cases with a death toll of 300,441, and the virus is now in 216 countries [3].
Based on experts’ opinions, The Economist reports a broad guess that 25-70% of the population of any infected country may catch the disease and that the virus could kill 60,000 Americans in a worse-scenario year when the death toll could be in the millions across the world [4] and it has already been excessed in the United States with a death toll of 82,119, 27.33% of global deaths, and total confirmed cases of 1,361,522 [5]. In a more recently official guess, the White House forecasts the novel coronavirus death toll may be 100,000 to 240,000 despite the measures taken in the US [6] which is a new epicenter for the novel coronavirus.
Weapons to Fight Pandemics and COVID-19
Fighting tools for any pandemic may be classified into two categories in general which are also valid for the COVID-19 outbreak: pharmaceutical that are both treatment and protection instruments and nonpharmaceutical tools.
The pharmaceutical methods include vaccines and antiviral drugs. WHO says that, to date, there is no vaccine and no specific antiviral medicine to prevent or treat COVID-19 [7], and that globally more than 20 vaccines are in development, and several therapeutics are in clinical trials [8], indeed currently over 100 vaccines. It is well known that the availability of approved medications will take months when vaccines optimistically take a year.
Apart from vaccines and drugs, nonpharmaceutical interventions may cover basic personal protection tools such as frequently washing hands, hand hygiene[9], using facemasks and N95 masks and social mitigation strategies including social distancing, life style education like avoiding close contact and cover coughs and sneezes, and school closure as well as more strict measures like travel restriction, isolation and quarantine [10] and stay-at-home order.
Quarantine as it is now employed is a public health tool and a collective action for the common good. Modern quarantines are more likely to involve a few people exposed to contagion in a small area, such as at a hospital, on an airplane or at a public gathering, and only unusually are applied to entire cities or communities [11]. Although it is rare and new to science and modern applications to quarantine a whole city or country, which seems to be a ‘new normal’ in fighting epidemics. Some whole countries are on lockdown to contain COVID-19. The lockdown goes viral as the novel coronavirus does. One third of the world was/is on lockdown as if the planet earth has been closed.
As the novel coronavirus spreads, WHO calls on industry and countries to increase manufacturing of personal protective equipment such as N95 respirators, facemasks, gowns and gloves by %40 to meet rising global demand due to the COVID-19 and associated buying. There would be a global shortage to meet the demand even from frontline health responders.
All pharmaceutical and non-pharmaceutical fighting measures for all epidemics and as well as COVID-19 pandemic are already scarce resources and carrying costs, and thus naturally have limitations. In a nutshell, fighting costs and constraints are always matter for any epidemic, outbreak, pandemic or bioterror attack.
We propose two mathematical programming models for fighting any pandemic at micro and macro levels, respectively; the first one is personal protection model or protocol and the other one is mass protection model for a country. We also apply these theoretical models to coronavirus pandemic with real-world data for an American and the United States of America. This work on fighting pandemics and coronavirus [12] is published in European Journal of Pure and Applied Mathematics on 28 April 2020.
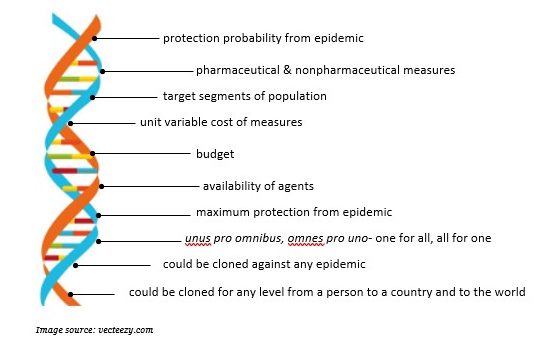
Our models directly focus on optimal protection rather than forecasting cases and deaths, independent of numbers of cases and deaths, apart from common mathematical epidemiological models. Based on a metaphor, in our approach, we set the DNA of fighting pandemics in general and the DNA, the genetic material of our models, could be cloned and applied to fight any pandemic, epidemic or bioterror attack for anyone and any country at any time.
Personal Protection Protocol
We develop a personal protection model or protocol that maximizes total protection probability of a person subject to required number of tools and budget constraint. The recipe that is a binary nonlinear programming model is given in detail in [12].
We also implement the model with real-world data for a person living in USA to obtain optimal protection strategies from COVID-19. The person is an adult aged between 18 and 59, and can work from home. Although the model can handle any finite number of tools, we consider a vaccine and two antiviral medicines as pharmaceutical tools and using surgical mask, N95 respirator, hand hygiene products, lifestyle adaptation, 50% social distancing and self-quarantine as nonpharmaceutical interventions for the adoption of the person for 6 weeks.
We employ either-or constraints for the model so that the person cannot adopt vaccine and any antiviral or both antivirals at the same time. The data acquisition for this one-person model is also presented in [12].
According to our personal protection model, the person should adopt vaccine, surgical mask, hand hygiene, lifestyle education and self-quarantine strategies for 6 weeks within his/her $500 budget. S/he should stay at home and work from home for 6 weeks after getting vaccine and use hand hygiene products and surgical mask with careful lifestyle like avoiding close contact and cover coughs and sneezes. This optimal protection strategy provides 99.991% protection of the person with a cost of $416.224. The costliest strategy is self-quarantine with 81% share of cost.
There are no approved vaccine and antivirals for COVID-19 at present. Thus, based on the current practice, we easily re-run the model without pharmaceutical tools, we get an optimal solution again under new conditions covering only some nonpharmaceutical interventions. In this case, the optimal protection rate reduces to 99.910%. The protection gap is 0.08% which is the opportunity cost of vaccine or antivirals.
Mass Protection Model
We propose a nonlinear integer programming model that maximizes mass weighted protection probability of people from an epidemic, pandemic or bioterror attack under some certain scarce resources, functional constraints and budget. The model could work at the levels from county to city, to state and across country as well as in the global scale. Our mass fighting model is inspired by the weapon-target assignment problem.
We segment whole population into medical protection targets of sub-populations, and partitions of target segments are persons in the model language as well. Those target segments may be chronic patients, pregnant women, health care workers, infants and other specific groups, and the remaining people. Our weapons are treatment and protection instruments; pharmaceuticals such as vaccines and antiviral drugs and nonpharmaceutical tools including use of surgical masks, N95 respirators, hand hygiene products, airlines cancelling, voluntary self-quarantine and lockdowns. In this work, a priori tools are designated as the tools that have been previously decided for adopting. As instance, quarantine regions, border shutdown, airline cancelling, and cancelling sailings may be previously decided for implementation. Their decisions are independent of the model, but affects the model components. In the model, we assume the contributions of the people characterized by a priori decisions to related target segments are only compactly represented by their segment protection probabilities. Also, an agent means an appropriate one of a person, a unit or quantity of dose. The model outputs can be implemented during a planning horizon.
The model assigning appropriate agents to target segments of population determines that who should adopt which measures at what level for maximum mass protection. The formulation and details of the model as well as data acquisition for coronavirus pandemic are also given in [12].
Mass Protection Policy for Fighting COVID-19 in the United States
We run the mass protection model with real data of USA to protect the whole country from COVID-19. Even though the model can handle thousands of target segments and therapeutic/nontherapeutic and pharmaceutical/non pharmaceutical tools; any finite numbers of tools and targets (), we consider 14 tools and 9 target segments of USA population. The planning time horizon is 6 weeks.
The pharmaceutical tools are a vaccine and two antiviral medicines when nonpharmaceutical instruments are use of surgical masks, N95 respirators and hand hygiene products, lifestyle adaptation, school closures, 50% social distancing, voluntary self-quarantine and a set of a priori tools including that a city with a population of 4,150,000 must be on lockdown.
We set the target segments of the US population as chronic patients, pregnant women, health care workers (HCWs), infants (0-6 month), and people aged 6 month-14 years, 15-24 years, 25-54 years, 55-64 years and 65+ years. In this study, we consider chronic patients, pregnant women, health care workers and older people (65+) as risk factors.
According to the solution of the mass protection model, presented in detail in [12], 99.431% of HCWs, 94.707% of chronic patients, 99.741 of pregnant women, 99.223% of aged 65+ and, etc. are protected from COVID-19 if the near-optimal policies are adopted. The average protection ratio or average protection probability of all target segments is 96.961% which is very high. The top four weighted protection values are of HCWs, aged 65+, chronic patients and pregnant women which are all risk factors. The costliest segment is chronic patients with a share of 45.06% of total cost when the least costly is infants (0-6 month) with 0.56%.
The costs of tools are also obtained that the costly tool is voluntary self-quarantine with a share of 34.479% of total cost as the pharmaceutical tools are associated with 2.469%. we also observe that all available agents are assigned to target segments. The total cost of near-optimal assignment is $ 293,332,400,284 which is less than half of allocated total budget, and only 14.66% of $ 2 trillion that has been recently released by the US government and the US Senate to combat and protect from the novel coronavirus pandemic and economic devastation [13].
Mind the Gap: Opportunity Cost of Vaccines and Antiviral Medicines
There are no approved vaccines and antiviral medicines against novel coronavirus at present. Thus, for the present-day situation, we also re-run the mass protection model without pharmaceutical tools, only with the nonpharmaceutical tools by just easily giving zero protection probabilities to the vaccine and antivirals.
The average of protection probabilities of all target segments reduces from 96.961% to 94.198% as the total cost decreases by about $7,25 billion. The protection ratio gap between the models with and without vaccine and antivirals is 2.763% which corresponds the failure of protecting 8,292,109 people as much as population of the State of Virginia or New York City – opportunity cost of vaccines and antiviral drugs. If the available number of non-pharmaceutical agents would decrease or be in shortage in the nonpharmaceutical case, the number of expected unprotected people would increase dramatically.
Unus pro omnibus, omnes pro uno: Relation Between the Models
It could be asserted that “protecting yourself means protecting people” is an extremely important principle in epidemiology to combat the outbreaks. Our two proposed models for fighting all epidemics, pandemics or bioterror attacks in this work are in favor of the fact unus pro omnibus, omnes pro uno – one for all, all for one. From a standpoint, the mass protection model with integer decision variables is a mathematical generalization of the personal protection model with binary decision variables, and conversely, a special case of the mass protection model is the personal protection model. If you join the mass protection
policy, you will have personal protection strategy in a somewhat and if you adopt personal protection protocol, you will contribute to the mass protection policy to fight epidemics, which leads us to unus pro omnibus, omnes pro uno – one for all, all for one.
Recognize the Double Invisible Moving Enemy
As the moving enemy, novel coronavirus, is double invisible due to its viral nature and the availability of the high level of symptom-free cases of infected people which is guessed 1 in 4 in the US and 2 in 4 in Ireland, the seriousness and difficulty of fighting coronavirus pandemic should be internalized altogether.
Recognize the enemy, as protecting yourself means protecting people, love life, follow the rules that the DNA of fighting pandemics recommends and stay at home. Help save millions of lives. That is the greatest ever social impact!
REFERENCES
- Coronavirus Disease (COVID-19) Outbreak. https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (2020), 10.03.2020
- Coronavirus disease 2019 (COVID-19) Situation Report – 51. https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200311-sitrep-51-covid-19.pdf?sfvrsn=1ba62e57_6 (2020), 11.03.2020
- https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (2020), 16.05.2020
- The Economist. The Virus is Coming. The Economist, February 29th-March 6th 2020. https://www.economist.com/leaders/2020/02/27/the-virus-is-coming (2020), 05.03.2020
- Coronavirus disease 2019 (COVID-19) Situation Report – 116. https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200515-covid-19-sitrep-116.pdf?sfvrsn=8dd60956_2 (2020), 16.05.2020
- Leary A., Calfas J & Ping C.K. White House Projects 100,000 to 240,000 U.S. Coronavirus Deaths., https://www.wsj.com/articles/chinas-coronavirus-count-excluded-infected-people-with-no-symptoms-11585650226 (2020), 03.04.2020
- Is there a vaccine, drug or treatment for COVID-19? https://www.who.int/news-room/q-a-detail/q-a-coronaviruses (2020), 02.04.2020
- Centers for Disease Control and Prevention. What every individual can do to protect themselves and others. https://www.cdc.gov/coronavirus/2019-nCoV/summary.html#risk-assessment (2020), 05.03.2020
- Coronavirus disease (COVID-19) advice for the public. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/advice-for-public (2020), 06.03.2020
- Centers for Disease Control and Prevention. About quarantine and isolation. https://www.cdc.gov/quarantine/quarantineisolation.html (2020), 06.03.2020.
- Knobler, S., Mahmoud, A., Lemon, S., Mack, A., Laura, S.& Oberholtzer, K. (Editors). Learning from SARS: Preparing for the next disease outbreak: Workshop Summary, Forum on microbial threats, The National Academies Press, Washington, DC (2004).
- Çetin, E., Kiremitci, S. & Kiremitci, B. Developing optimal policies to fight pandemics and COVID-19 combat in the United States. Eur J Pure Appl Math. 2, 369-389 (2020). https://doi.org/10.29020/nybg.ejpam.v13i2.3700
- The US Senate. S. 3548 – Coronavirus aid, relief, and economic security act – CARES, Introduced in Senate on 19.03.2020, https://www.congress.gov/bill/116th-congress/senate-bill/3548/text (2020), 29.03.2020.
Eyüp Çetin (eyup.cetin@ejpam.com) is a professor of operations research and statistics. He formerly served as the founding dean of the Faculty of Transportation and Logistics and vice dean of the School of Business at Istanbul University. In addition, Çetin is affiliated with New York Business Global, USA. He is also founder & editor-in-chief of some prestigious journals.
Serap Kiremitci (serapy@istanbul.edu.tr) is an assistant professor of operations management in the School of Transportation and Logistics at Istanbul University. She holds a Ph.D. in operations management from the School of Business at Istanbul University.
Barış Kiremitci (baris.kiremitci@ejpam.com) holds a Ph.D. in operations research and is affiliated with New York Business Global, USA. He is also a trainee lawyer member of Istanbul Bar Association.
Suggested Citation:
Eyüp Çetin, Serap Kiremitci and Barış Kiremitci, The DNA of Fighting Pandemics: Cloned Against Coronavirus, 17 May 2020, New York Business Global Publishing, Maryland, USA.